INFECTION CONTROL / STERILIZATION & SANITATION

< QUICK SCROLL MENU
INFECTION CONTROL
BACTERIA
PIONEERS
LEVELS OF INFECTION CONTROL
ITEMS TO BE DISINFECTED
DISINFECTANT PROCEDURE
TYPES OF DISINFECTANTS & EQUIPMENT
PROPER HANDWASHING
INFECTION CONTROL
In the past when we talked about the subject that is now infection control we talked in terms of sanitation, decontamination, safety in the salon and bacteriology and we viewed them as separate entities. Logically speaking it makes extreme sense to merge them together. After all it is because of bacteria that we as professionals must effectively clean our work environment and the tools of our trade further; this must be done in a manner that ensures safety in the salon for all those concerned. Perhaps the best place to start in the subject of infection control is right where the need for control begins. The need to exhibit control is due to bacteria.
BACTERIA
Bacteria are one celled living micro-organisms so very minute that a microscope is needed to see them. Imagine if you can a pencil eraser. Now imagine, we line 1000 bacteria straight across the eraser, we would still have room to spare. If being tiny were not enough, with the correct conditions, bacteria have the audacity and capacity to multiply at a very rapid pace. We could have one bacterium cell at midday and due to the process of mitosis we would have sixteen million by midnight.
Scientists believe there are millions of different species of bacteria however only 4,500 have been identified to date and they are classified by two classifications; pathogenic and non-pathogenic. Fortunately 70% of bacteria are non-pathogenic (beneficial) but; unfortunately the 30% that are pathogenic (disease causing) can be very dangerous.
Let us first take a look at non-pathogenic bacteria. As stated earlier non-pathogenic are beneficial and harmless. They can be found in a number of places. The human digestive system is rich in beneficial bacteria that begin with the saliva in the mouth which is assisted by the salivary glands. The pepsin found in the stomach along with chymotrypsin and trypsin continues to break down the food that is ingested and broken down through the complex process of metabolism. This is just one example of the beneficial bacteria that are found in the human body.
Saprophytes are another example of beneficial bacteria. If given the choice of being placed in a room with a person that is experiencing an active cough and running nose or a dead animal that is covered in maggots; most people would take the choice of the person that is showing signs of illness. The best choice however; would be to opt for the dead animal. Yes there might be some unpleasant odors associated with this choice but the fact is the presence of the dead animal and the maggots offer no threat. The sick person however would be of concern as they are most likely contagious. The maggots are saprophytes and they are very important to our ecology. They live on dead or decaying matter/ organisms, where they obtain their nourishment and recycle organic material into the soil breaking it down into simpler compounds that can be used to nourish other sources i.e. the vegetables we eat or the grain that is eaten by livestock. So it can be said that saprophytes aid in decomposition and actually give back to the earth.
As beneficial as non-pathogenic bacteria are, pathogenic bacteria can be a disaster waiting to happen. Pathogenic bacteria may account for only 30% of all bacteria but it is because of the havoc they can evoke that infection control is imperative in every phase of life and is extremely important to the professional of every aspect of cosmetology.
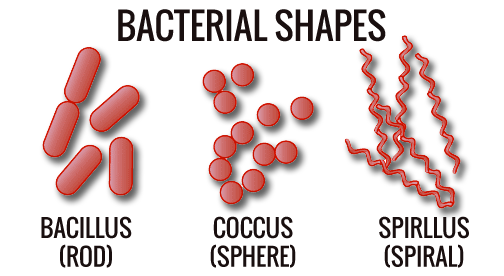
There are 3 classifications of pathogenic bacteria: Cocci, Bacilli and Spirilla we shall take a look at them individually.
- Cocci are round or spherical shape pus producers that grow singularly or in groups. Cocci will manifest in three forms: Staphylococci, Streptococci, and Diplococci.
- Staphylococci grow in clusters and are responsible for local infections such as boils, abscesses and pustules. Typically it is called a staph infection and infections of the skin are the most common however; pneumonia, food poisoning, toxic shock syndrome and blood poisoning are also common. Most staph infections are easily treated with antibiotics however; there are MRSA / Methicillin-resistant Staphylococcus Aureus which are resistant to common antibiotics. These bacteria are spread by direct contact or contact with contaminated items or surfaces. It is believed that at least 30% of the population carries the infection on their skin and in their nose.
- Streptococcus grows in strips or chains and is classified as Group A or Group B bacterium. Group A are responsible for such infamous infections like strep throat, necrotizing fasciitis (aka the flesh eating disease) and toxic shock syndrome. Many people actually have streptococci in their throat or skin and have no signs of illness and most of these infections are easily cured with antibiotics. What makes this bacteria life threating is when it has access to areas in the body where bacteria typically does not exist such as blood, muscle and lungs. Necrotizing fasciitis is aggressive and can rapidly destroy muscle, fat and skin tissue. STSS or streptococcal toxic shock syndrome (not to be confuse with staphylococcus aureus which is associated with tampon usage) can cause rapid drop in blood pressure and the result can be organ failure (typically kidney, liver, or lungs).
The spread of these bacteria comes from direct contact of nose or throat mucus from persons that are infected. Direct contact with infected wounds and sores are the cause for cross contamination. Persons that are infected are much more likely to spread the infection than those who have no symptoms or evidence of infection. Annually there are approximately 9000 to 11,500 cases of invasive Group A Streptococci compared to several million cases of strep throat and impetigo.
- Group B Streptococcus is sometime referred to as “baby strep” and is the cause of blood infections, pneumonia, skin, soft tissue, bone and joint infections. It is the leading cause of meningitis. The Center for Disease Control recommend that all pregnant women in their 35th to 37th week be tested for GBS because 25% of pregnant women carry the bacteria in their rectum or vagina and the rate of infection very high in newborns. GBS can occur in all age groups and the rate of occurrences increases with age. These bacteria can come and go in the human body without any symptoms, or it can cause mild infections such as urinary tract infections. The transmission of this bacterium is uncertain however; since GSB is a common organism in the gastrointestinal, this may be the source.
- Diplococci commonly grow in pairs and are responsible for pneumonia and pneumococcal meningitis.
- Bacilli most often applies to any rod like bacteria most commonly found in soil and water. When conditions are unfavorable it can easily form spores that are resistant to heat, chemicals and sunlight which allows them to stay dormant for long periods of time. Fortunately most are not harmful to humans with the major exceptions of bacillus anthracis causing anthrax (human contact with animals) and bacillus cereus that causes food borne illnesses (food that is improperly cooked or stored).
- Spirilla the third distinct bacterial cell shape that twist and turn like a spiral. It is most common for its responsibility in the sexually transmitted disease syphilis (treponema pallidum) and lyme disease (borrelia burgdorferi).
There are other pathogens that give cause for concern:
Viruses are many times smaller than bacteria and can actually infect bacteria. Unlike bacteria they need a living host in order to live and thrive. Viruses cause such nasty diseases like chicken pox, measles, mumps, influenza and the common cold. As we well know these ailments can be easily spread through casual contact. Viruses can also prove to be deadly in severe cases of influenza, hepatitis, HIV and AIDS just to name a few.
Fungi can be either beneficial or harmful. Fungi are devoid of chlorophyll and therefore cannot photosynthesize so it must absorb nutrients from organic matter produced by other organisms. Most fungi live on dead matter (saprophytes) and a small few live off organic matter (parasites). Parasites can be either plant or animal and unlike saprophytes are never beneficial to anything but themselves. They can invade the body’s tissues either externally or internally and cause disease.
PIONEERS
The world of germs is nothing new and pathogens have been creating havoc for centuries and scientist have been studying them for almost as long. There are some pioneers and heroes in this war on pathogens that we must pay homage to.
-
Girolamo Fracastoro was an Italian physician as well as an astronomer and geologist. Of all the hats Fracastoro wore perhaps those of physician and scientist were the most important. Born in Verona Republic of Venice, in the year 1478 he proposed the “germ theory of disease” some 300 years, before it was formulated by Louis Pasteur and Robert Koch. Fracastoro was also responsible for studying and naming the syphilis disease in 1530. In 1546 his Concept of Epidemic Disease was told in a piece published on Contagion and Contagious disease which stated that each disease was caused by an individual type of rapidly multiplying germs that was spread or transferred from the infector to the infected by direct contact through the air, and on such items as clothes and linens. This concept was not completely new as 1st century Roman scholar Marcus Varro believed that micro-organisms were the cause of disease. When Fracastoro first announced his concept it was greatly accepted and there was much excitement surrounding it however it soon fell into disrepute and acceptance waned until the experiments in the 1800’s turned concept into fact.

- Agostino Bassi (1773 – 1856) an Italian entomologist whose love for biology placed him on a 25 year journey to aid silk farmers in 1849 and discovered that fungus and its spores were the cause of their devastation. Perhaps one of his most important contributions was his recommendation for the use of disinfectants and cleanliness. His work explained that many diseases whether plant, animal or human were caused by pathogenic organisms.

- A pioneer in the field of microscopic anatomy and pathology, Friedrich Gustav Jacob Henle (1809 – 1885) drew his work on the achievements of Agostino Bassi and actually laid ground work for future scientists and physicians. His publication “Von den Miasman und Kontagien” (On Miasmata and Contagia) in 1840 revisited and reaffirmed the concept that micro-organisms were the reason for many diseases and the morbid matter, in relations to communicable diseases increases in amount in the host after a period of incubation. Further his work set the stage for his student Robert Koch.

Probably one of the greatest bacteriologists to live is 1905 Nobel Prize winner Robert Koch (1843 – 1910). His accomplishments are many but, the most prevalent to the cosmetology industry are the isolation and identification of anthrax bacillus in 1876 and tubercle bacillus in 1882. Koch was appointed Professor of Hygiene and Bacteriology at the University of Berlin where he researched bacterial diseases in humans and animals. He was fundamental in the development of a whole generation of medical scientist and bacteriologist in a wide range of fields and studies.
With the collaboration of Jacob Henle he developed the Henle – Koch postulates of 4 criteria required to prove a micro-organism caused a disease:
- Organism can be isolated in case of the disease.
- It can be cultivated in pure culture.
- Cultured organisms can induce the disease in experimental animals.
- The organism can be recovered from the infected experimental animals.

Louis Pasteur (1822-1895) was an amazing French biologist and chemist, he is one of the worlds most celebrated scientist. Convinced of “the germ theory” (belief that infectious diseases are caused by micro-organisms), he was bound and determined to take his knowledge of science and discover a way to help people live healthier lives. His contribution to medicine, chemistry and biology proves that he was successful in his ambition.
Known as the “father of pasteurization” it was through his efforts to help French winemakers succeed in delivering un-spoiled wine to buyers, he discovered that heating the wine would not change the taste but would kill early bacteria. Hence the process of pasteurization was born. He customized some of the applications of pasteurization to accommodate its use in other foods.
Due to his insistence that infectious diseases were a product of micro-organisms he led other scientists to pursue and conquer sterilization, disinfection, vaccines and in the 19th century antibiotics. Pasteur himself developed vaccines for rabies and anthrax as well as treatments for tetanus, tuberculosis and diphtheria.
As reward for his many contributions to ensure the possibilities of healthy living the Louis Pasteur Institute was created through international funds in 1888. In keeping with his resolve to study micro-organism; the institute continues to research microbiology and immunology. It has made vast contributions to eradicate HIV.
Famed British surgeon and scientist Joseph Lister, born April 5, 1827, developed methods that changed the practice of surgery and medicine forever and his methods eventually trickled into the industry of cosmetology.
After witnessing the death of 40 -50% of amputation patients due to sepsis he first theorized that perhaps airborne dust maybe the cause. He soon learned of the work of Louis Pasteur in regards to infectious micro-organisms and decided to use phenol as an antiseptic. Prior to this ground breaking act surgeons and their assistance were not required to wash their hands. As a matter of fact, dirty laboratory coats were seen as a sign of knowledge and experience and the stench was referred to as “good surgical stink”.
An earlier discovery by Friedlieb Runge (1797 – 1867) of creosote which was later turned into carbolic acid would prove crucial to Joseph Lister’s work. Dr. Runge’s work as a chemist led him to discover many coal tar products (creosote and phenol are some of its byproducts). Early uses were the treatment of wood used for the railway ties and ships (to retard decay), sewage in England and to fight parasites and manage odors during cholera and cattle plagues.
Building on Dr. Runge’s findings Dr. Lister started spraying his surgical instruments and surfaces with a solution of phenol. He also washed his hands in the solution and even used diluted portions to swab surgical and accidental wounds. Within 4 years the mortality rate was reduced by 15%. His discovery also was credited for increasing the safety for both mother and child during child birth.
The number of infections was greatly reduced in hospital settings and eventually in other area such as food handling and general house cleaning. This is why Joseph Lister is “the father of modern antisepsis”. In 1879 the mouthwash Listerine was name in his honor as well as the bacterial genus “Listeria”.

Last but, not least of our pioneers and the only women acknowledged here is Sarah Breedlove (1867-1919) a.k.a. Madame C.J. Walker. A pioneer in more ways than one she grew a business that she started in her kitchen into a multi-million dollar business, making her the first female self-made millionaire in American history. Though not formally educated Madame Walker’s business acumen allowed female entrepreneurs across the nation to improve their economic situation.
After successfully formulating a concoction to restore her hair after losing it to damaging hair care products and the stress from being widowed at age 20 (she was probably suffering from a form of alopecia), she was approached by many who witness the transformation of her hair. She began teaching women how to use the product and sell the product and service. This created such a demand that she soon had to create a strict protocol for her team of followers to adhere to. It was her desire to perform hair care services in a sanitary manner to ensure that no harm would come to her patrons. Many states began adopting her practices and actually used much of her protocol in state laws and regulations.
LEVELS OF INFECTION CONTROL
There are three levels of infection control and they are Sanitation, Disinfection and Sterilization. Sanitation is the lowest level of infection control, but it is important to understand that though it may be the lowest it is not the least important. In the fight against pathogens it is probably the most important. If sanitation is not performed disinfection or sterilization cannot be achieved.
Sanitation allows for the physical removal of debris (i.e. hair from combs and clippers, dead cut skin from cuticle nippers and body fluids from comedome extractors) and is performed on items that are deemed non critical. Non- critical; meaning that the item is used on unbroken skin. Sanitation is the first step in the process of protecting the professional and their clients from the unnecessary transmission of disease.
Next in line for defense against pathogens is disinfection. Disinfection is accomplished with the use of chemicals rendering most pathogens inert. However; it allows bacterial spores to survive which if not addressed can lead to contamination. In most salon settings and situations disinfection is the highest level of infection control necessary as the implements in use are typically semi critical.
When more effective measures are needed the highest level of infection control is implemented. Sterilization will kill everything. It does not discriminate as it does not recognize the difference between pathogenic agents and nonpathogenic agents. Also it will destroy those bacterial spores that disinfection procedures leave behind. Sterilization practices can be labor intensive and costly and though not necessary for non- critical or semi- critical it is reserved for critical items
Items to be Disinfected
In all of the areas of cosmetology whether it is hairdressing, facials or a polish gel, service tools are used that are either characterized as non-critical, semi-critical or critical items. Determining the difference of the three is crucial. Non-critical items are used with the intention of coming into contact with only unbroken skin. Unbroken skin is the first line of defense against pathogens and acts as a barrier. For this reason non-critical items only need to be sanitized. Examples of Non-Critical Items:
Countertops
Magnifying Lamps
U.V. Lamps
Hands
Semi-critical items are intended to or may have a likely chance of coming in contact with broken skin or mucous membrane. With those intentions these items require disinfection with a high level, broad spectrum, hospital grade disinfectant.
Examples of Semi-Critical Items:
Tweezers, Combs, Cuticle nippers.
Unlike non-critical and semi-critical items, critical items are designed and intended to come in contact with blood, body fluids and other tissue therefore; it is required that if these items are not disposable (disposable is preferred ) they must be sterilized. As per their design; no critical items are used in the cosmetology profession.
Lancets
Electrology needles
DISENFECTANT PROCEDURE
- Clean with soap and water (removing all debris)
- Rinse and dry with clean towel or paper towel
- Completely immerse in hospital level or EPA approved disinfectant
for 10 minutes or required time of manufacturer.
- Remove items from wet disinfection container with tongs, basket or gloved hands.
- Rinse and dry.
- Store in clean, closed container.
Per CHAPTER 61G5, Florida Administrative Code -61G5-20.002
Salon Requirements – Disinfecting methods which are effective and approved for salons: First, clean articles with soap and water, completely immerse in a chemical solution that is hospital level or EPA approved disinfectant as follows:
- Combs and brushes, remove hair first and immerse in hospital level or EPA approved disinfectant;
- Metallic instruments, immerse in hospital level or EPA approved disinfectant;
- Instruments with cutting edge, wipe with a hospital level or EPA approved disinfectant;
- Implements may be immersed in a hospital level or EPA approved disinfectant solution.
- Shampoo bowls, facial beds and neck rest, clean and disinfect between each use.
- All disinfectants shall be mixed and used according to the manufacturer’s directions.
- Ultra violet Irradiation may be used to store articles and instruments after they have been properly cleaned and disinfected.
- For complete guidelines for pedicure unit cleansing and disinfecting please refer to 61G5-20.002 Salon Requirements.
TYPES OF DISINFECTANTS AND EQUIPMENT
Disinfectants are strong and powerful chemicals that must be respected and used correctly. When used correctly disinfectants can destroy pathogens on contaminated implements and surfaces. If used incorrectly they can be quite dangerous.
DISINFECTANTS
- Quaternary Ammonium Compounds or commonly called Quats are very safe and highly effective when used properly. Quats are widely used as disinfectants and make good cleaning agents. Typically they are sold as hospital disinfectants as they are fungicidal, bactericidal and virucidal. Most formulas contain rust inhibitors making them even more appealing to salon professionals along with its typical disinfection time of 10 minutes. REMEMBER to always follow manufacturer’s instructions.
- Bleach 5.25% sodium hypochlorite (household bleach) can be an effective disinfectant however; it is a strong corrosive chemical. It can easily cause damage to plastics, rubber and metals. On the human side it can irritate eyes, skin and the respiratory track. Bleach has been strongly linked to breast cancer. When using bleach always follow manufacturer’s instructions and remember that OSHA requires that gloves and mask be worn. Bleach solution is an unstable mixture and cannot be saved from one day to another.
EQUIPMENT
Personal protective equipment (PPE) are items that are worn to eliminate or reduce one's exposure to hazardous chemicals. They include: Gloves, goggles, protective clothing and even respirators.
ANTIBIOTICS and their MISUSES
Another element in infection control that typically gets little attention in our industry is antibiotics. By definition, antibiotics are drugs used to treat bacterial infections. They are produced by living organisms with attention to bacteria and fungi with intention to kill or prevent the growth of harmful pathogens. What is important to mention is; antibiotics have no effect on viral infections.
Antibiotics have become a staple in the world of medicine. Most of the populous takes the existence of antibiotics for granted as something that has always been and will always be. This attitude in a sense has jeopardized their usefulness.
The need for antibiotics has been recognized for thousands of years. Historians and scientists show evidence that ancient civilizations used molds, plants, warm soil, frog bile with sour milk, turtle shells, snake skins and oil cakes (just to name a few) in the fight against infections.
Modern history gave the world even more promise with research and experimentation by various scientists. As early as 1640, John Parkington recommended the use of mold for treatment in his book on pharmacology and by 1932 another massive breakthrough was achieved when Gerhard Domagk discovered sulfonamidochrysoidine which was the first antibiotic on the market. In between these two amazing discoveries were many great works and accomplishments, one being Louis Pasteur’s discovering that bacteria could kill another bacteria (anthrax bacilli).
Perhaps one of the most important is Sir Alexander Fleming, in 1928 he discovered lysozyme a powerful enzyme that prompts the breakdown of certain carbohydrates housed in the cell walls of certain bacteria. Much by accident Sir Fleming upon cleaning his cluttered laboratory realized that a glass plate previously covered with staphylococcus contained mold in the shape of a ring, within the ring the glass plate was bacteria free. This mold was penicillium notatum. It would be another 10 years before the bacteria killing substance would be isolated and named – penicillin. This was done through extensive research by Howard Florey and Ernst Chain at Oxford University. Florey successfully commissioned an American drug company to mass produce the penicillin and its usage was first confined to the U.S. Military and was nicknamed “the wonder drug”. In 1945, Fleming, Florey and Chain were awarded the Nobel Prize for Medicine. Post 1945 was deemed the era of antibiotics and in 1947 antibiotics were available to the U.S. masses.
Since their introduction antibiotics have transformed medicine by treating and preventing infections and protecting individuals with compromised immune systems. They have promoted growth and prevented disease in livestock and other food animals. Their existence has been both lifesaving and life changing. Unfortunately, the overuse of these “wonder drugs” has caused once treatable infections to become hard to treat and cure. Our “wonder drug” is less than 100 years old and is becoming less effective and our arsenal is dwindling!
Overuse is not limited to the unnecessary prescriptions being written by physicians but; can also be attributed to its massive misuse in poultry, cattle, swine and fish – which harbors significant populations of antibiotic resistant bacteria. The bacteria are then transmitted to humans through their meat, eggs and milk.
Driven by prosperity and population growth, demand for animal protein is at an all-time high and farmers, in an effort to satisfy demand are using antibiotics to cure disease, prevent disease/infection and controversially to promote rapid growth. In 2010, according to the Center for Disease Dynamics, Economics and Policy (CDDEP) estimated that 63,200 tons of antibiotics were consumed by livestock.
The CDC credits antibiotic resistance for more than 2 million infections and 23,000 deaths each year in the U.S., with cost totaling approximately $55 billion.
Antibiotic resistance is a major problem and it is in our best interest as a society to preserve antibiotic effectiveness. This can be achieved by the following practices:
- Antibiotics only prescribed and taken when absolutely needed.
- When prescribed and dispensed antibiotics should be taken as prescribed with adherence to dosage and duration.
- Reduce need for antibiotics through proper sanitation and immunization.
- Reduce and eventually eliminate antibiotic usage in agriculture.
- Educate health professionals, policy makers and the public on sustainable antibiotic usage.
A national campaign for awareness on the misuse of antibiotics and the consequences is needed to draw attention to this universal problem and promote conversations for changes by and through our politicians, law and policy makers.

PROPER HANDWASHING
The Center for Disease Control says that the single most important act that anyone can do to limit the risk of transferring pathogens is hand washing. The recommended method of hand washing is listed below.
- Wet your hands with clean, running water (warm or cold) and apply soap.
- Lather your hands by rubbing them together with the soap. Be sure to lather the backs of your hands, between your fingers and under your nails.
- Wash your hands for at least 20 seconds. Sing or hum the ” Happy Birthday “ song from beginning to end twice.
- Rinse your hands well under clean running water.
- Dry your hands using a clean towel or air dry them.
- Before, during, and after preparing food.
- Before eating food.
- Before and after caring for someone who is sick.
- Before and after treating a cut or wound.
- After using the toilet.
- After changing diapers or cleaning up a child who has used the toilet.
- After blowing your nose, coughing, or sneezing.
- After touching an animal, animal feed or animal waste.
- After handling pet food or pet treats.
The following is a list of when the CDC says handwashing is required:
SUMMARY
Due to the many pathogens, it is necessary to exercise good and proper infection control measures. As we see, over the ages by way of dedicated and determined individuals from various branches of science and medicine we have acquired a better understanding of these disease producing micro-organisms. Understanding their structures, growth patterns, growth cycles and vulnerabilities, we know which level of infection control is needed to render a safe environment for our clients and ourselves.
Proper implementation of cleaning and disinfecting along with proper handwashing is paramount in reducing the spread of contamination, disease and the need for antibiotics.
WORKS CITED
Bailey, Diane Carol, Milady Standard Natural Hair Care and Braiding.Clifton Park: Cengage Learning, 2014
Cartwright, F. F. (n.d.). Joseph Lister, Baron Lister. Retrieved April 16, 2016, from http://www.britannica.com/
Ullmann, A. (n.d.). Louis Pasteur French Chemist and Microbiologist. Retrieved April 16, 2016, from http://www.britannica.com/
Agostino Bassi - Italian Bacteriologist. (n.d.). Retrieved April 16, 2016, from http://www.britannica.com/
Friedrich Gustav Jacob Henle – German Pathologist. (n.d.). Retrieved April 16, 2016, from http://www.britannica.com/
Stevenson, L. G. (n.d.). Robert Koch German Bacteriologist. Retrieved April 16, 2016, from http://www.britannica.com/
Madam C.J. Walker American Businesswoman and Philanthropist. (n.d.). Retrieved April 16, 2016, from http://www.britannica.com/
Health and Hazards in Nail Salons. (n.d.). Retrieved April 17, 2016, from http://www.osha.gov/
Personal Protective Equipment for Infection Control. (n.d.). Retrieved April 17, 2016, from http://www.fda.gov/
Antibiotics: MedlinePlus. (n.d.). Retrieved April 17, 2016, from http://www.nlm.nih.gov/medlineplus/antibiotics.html
(2016). Retrieved April 17, 2016, from http://www.cdc.gov/mrsa
The State of the World Antibiotics 2015. (n.d.). Retrieved April 17, 2016, from http://www.cddep.org/
History of the Development of Antibiotics. (n.d.). Retrieved April 17, 2016, from http://www.encyclopedia.com/
Hoyle, B. D. (n.d.). Bacterial Biology. Retrieved April 17, 2016, from http://www.encyclopedia.com/
Board of Cosmetology. (n.d.). Retrieved April 15, 2016, from http://www.myfloridalicense.com/dbpr/pro/cosmo/statutes.html
When and How to Wash Your Hands. (2016). Retrieved April 17, 2016, from http://www.cdc.gov/
